Scarring Alopecia: Clues that You’re Off Track and How to get back On Track
Scarring alopecias are hair loss conditions that have the potential to cause permanent hair loss. Patients often have scalp itchiness and may also expeirence burning in the scalp as well. Increased shedding is common. There is a lot of misinformation about these conditions becasue all too often they are grouped in the bigger category of ‘hair loss.’ It’s too often felt that what worked for one person with hair loss should work for another person. That’s just not the case if that other person has scarring alopecia.
After treating many patients with scarring alopecia over the years, I can say that there are often signs that that tell me that a patients needs a bit of help with how they are approaching their own scarring alopecia. These may be patients who contact our office, or patients who post concerns on social media or patients who come to the office.
Treating scarring alopecia is not only about connecting patients with effective treatments but also about dispelling myths and misinformation – some of it quite strongly rooted in the mind of the patient and sometimes their doctors too. Treatments can help the patient but knowledge also heals too.
Here are these 10 signs.
CLUE 1: The patient has no idea what they should be monitoring.
Many patients with scarring alopecia tell me that they leave their doctor’s office with prescriptions but don’t know exactly what they are supposed to be monitoring until their next appointment. Alternatively (as in CLUE 3 below), they leave the office with the expectation that their hair will grow back.
Patients with scarring alopecia should be monitoring SEVEN main things at home – scalp itching, scalp burning, scalp tenderness, scalp redness, scalp pimples (pustules), hair shedding and density in various areas of the scalp. Of course, not all patients want to monitor these things and leave it up to the doctor to ask about these things at the follow up appointments.
CLUE 2: The patient knows what to monitor but does not know how soon to expect it all occur.
Some patients come to understand the basics of what sorts of things they should be monitoring at home. They know to keep track of scalp itching, scalp burning, scalp tenderness, scalp redness, scalp pimples (pustules), hair shedding and changes in density in various areas of the scalp. However, they are not sure when all this is expected to improve or when they are to notice a change.
It is import to review these sorts of things with the dermatologist as they may differ slightly with the exact type of scarring alopecia. I normally expect scalp symptoms to improve within 2-3 weeks and scalp shedding to improve within 2-3 months. Changes in hair density however, may take 2-7 months depending on the type of treatment that the patient has chosen.
For lichen planopilaris, for example, these changes might occur as follows (according to various treatment)
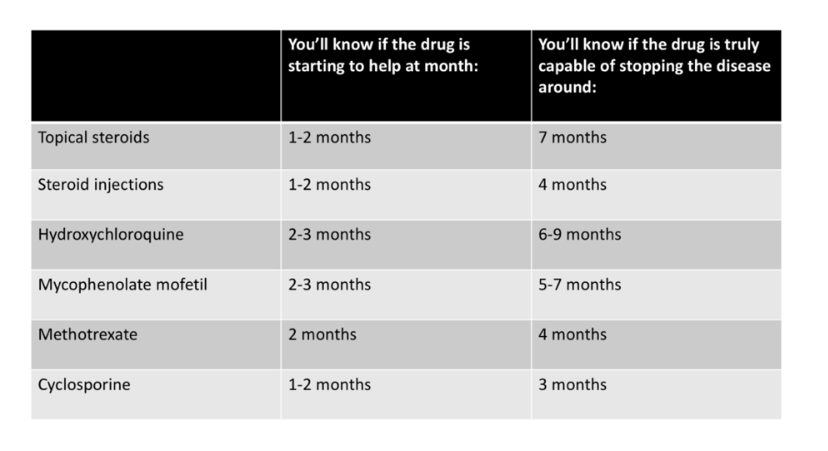
CLUE 3: The patient is expecting hair regrowth.
Many patients with scarring alopecia tell me that they have been doing all the things that their doctor recommended but are just not seeing an improvement. These patients are essentially telling me that they have not been educated on what it is they should expect.
While it’s true that hair regrowth does occur in many scarring alopecias, especially when treated in the early stages – the expectation should be that we STOP further hair loss rather than get new growth back. I tell patients that if they look the exact same as they do today in 6 or 12 months from now – it means the treatment is working well. Of course, I also tell some patients that a bit of regrowth might occur too. But this does not happen for everyone.
CLUE 4: The patient has never taken a photo of the hair & scalp to date.
If a patient has scarring alopecia and has never every taken a photo of the scalp since their diagnosis, they are missing out on an important step. Patients simply MUST take photos at home for optimal management. Of course, the doctor should take photos in the office but not all do. In today’s busy world, patients simply must be their own advocate and must take photos themselves or get someone else to take them.
When a patient of mine emails our office and says they are doing worse, the first thing I want to see is photographs.
Photos should of course be taken of the areas of hair loss, but should also be taken of normal appearing areas in the event these are slowly changing or in the event loss occurs in the future.
A patient who has never taken photos of their scalp needs to be educated on the importance of this step in scarring alopecia.
CLUE 5: The patient is shampooing the hair less and less.
Most patients with scarring alopecia react to their hair loss by shampooing less often. Many of these patients develop worse and worse seborrheic dermatitis on account of shampooing less and less. Some even develop thick scale in areas (pityriasis amiantacea) that traps bacteria and other microorganisms and worsens inflammation. In addition, some patients who shampoo less and less start to see more and more hair coming out after showering which prompts them to shampoo the scalp even less. A vicious cycle sometimes develops. For example, a patient who shampoos the hair once per week is going to see a lot more hair loss compared to if they shampoo the scalp daily.
I recommend that patients with scarring alopecia be gentle on their scalp but generally speaking shampooing every 2-3 days is appropriate for those with fine or straight hair and shampooing every 4-6 days is appropriate for those with curly hair. If seborrheic dermatitis is present, an anti-dandruff shampoo should be added to the shampooing routines. It thick scale is present, a salicylic acid based shampoo may be needed to help lift the scale.
CLUE 6: The patient has never used a topical corticosteroid.
Corticosteroids are the mainstay of treatment for many types of scarring alopecia. That’s not to say by any means that they are the most effective treatments. Not at all. However, for most types of scarring alopecia, especially lichen planopilaris, frontal fibrosing alopecia, discoid lupus, pseudopelade, they are a an improtant treatment to consider given their relatively safety and reasonable effectiveness.
A patient who has never used a topical steroid is quite likely to be misinformed, or poorly educated about their scarring alpecia. On average. Of course, there are exceptions. Yes. But we are talking averages here. A patients who has used this supplement or that supplement in hopes it will help their scarring alopecia or done this cosmetic non sense or that cosmetic non sense but has never used a topical steroid is all too common.
The purpose of this article is to help patients and physicians recognize the clues of being off track with treating scarring alopecia – and this is certainly one of them.
CLUE 7: The patient has never had any blood tests after your diagnosis.
Many scarring alopecias are diseases of the immune system of the body. Yes, it’s true many just have effects in the scalp (and the rest of the patient is perfectly healthy. But not all. We know that many scarring alopecias are associated with an increased chance of having blood test abnormalities – including thyroid abnormalities and low vitamin D. If a patient has not had blood tests since their diagnosis, they need them. Plain and simple. The basic tests are CBC (blood counts), TSH (thyroid studies) and ferritin (iron storage) and 25 hydroxyvitmain D (vitamin D status). Yes, other tests might be needed too – but these are the four basics that everyone needs. If a patient has never had blood tests, they are not quite on track yet.
CLUE 8: The patient has not seen a dermatologist to date about the hair loss.
This one often prompts some to take offence, but it should not. Many physicians treat hair loss and do a great job. Many hair transplant surgeons treat hair loss and do a great job. Many endocrinologists treat hair loss and do a great job. Many trichologists treat hair loss and do a great job. But most scarring alopecias are best handled by dermatologist.
A hair transplant surgeon, general practioner, endocrinologist and trichologist are not equipped with the tools to fully battle this group of diseases. A hair transplant surgeon does not usually prescribe systemic medications. For example, it’s rare that a hair transplant surgeon prescribes hydroxychloroquine, mycophenolate, cyclosporine, isotretinoin, clindamycin, rifampin. Are these really needed sometimes? They most certainly are.
A hair transplant surgeon treats hair loss with surgery and surgery is never ever an option in the early stages of scarring alopecia. An endocrinologist may have great strategies for some cases of female pattern androgenetic alopecia and may offer minoxidil, spironolactone and other systemic hormonal based options. But no, most endocrinologists don’t prescribe systemic medications for scarring alopecia and do not have the experience to monitor these systemic medications in the setting of scarring alopecia.
I’ll leave this topic now, but it’s one I feel strongly about. The only physician group with advanced skills to battle scarring alopecias are dermatologists. The exception of course would be physicians with advanced training in the field of hair loss dermatology. It’s simple. Yes, this concept rubs some the wrong way. But it shoud not. Patients are confused with available treatments. Bold statements are needed to help patients. And my primary concern is to help patients. The vast majority of patients with scarring alopecias are best treated by a dermatologist.
CLUE 9: The patient is using treatments but does not know what ingredients they contain.
It’s common for a patient to tell me they are using this treatment and that treatment. This vitamin and that vitamin. Many go on to say they are using something their hairdresser gave them or something they ordered from the internet, but they are not sure what it is.
If a patient is using something that they don’t know what it is, they need to stop. The treatment of scarring alopecia is a finely tuned process. At every single step, we need to know what we are doing. Taking things that one does not know what it contains is unsafe.
The immune system however, does know what the patient is taking – and so does the rest of the body. Some treatments activate the immune system, some have no effect and some actually weaken it. This includes natural products, herbs and random supplements.
CLUE 10: The patient is buying more and more products from the internet.
Patients who find themselves buying more and more treatments from the internet are probably not on track. This supplement, that supplement – it probably does nothing in the case of scarring alopecia. Fancy packaging and elevated prices are not associated with a great chance of helping scaring alopecia.
Do I ever recommend various supplements? Sure. Some may have benefit in non scarring alopecias, especially those associated with increased shedding (telogen effluvium). Rarely do they help scarring alopecia.
If a patient is increasing turning to amazon or various online website stores for options for their hair loss, it’s probably an indication that they should be seeing a dermatologist who treats scarring alopecia.
Conclusion and Summary: How do I get back on track?
There is a great deal of misinformation about scarring alopecias out there in the world. After treating many patients with scarring alopecia over the years, I can say that there are often signs that that tell me that a patients needs a bit of help with how they are approaching their own scarring alopecia.
I feel strongly that patients need to know what it is they should expect and how best to monitor their scarring alopecia. Not everyone follows there symptoms like our chart enables them to, but I certainly encourage patients to take photos. Everyone with primary scarring alopecia needs blood tests and there simply are no exceptions. Some types of scarring alopecia may need more tests than others, but everyone needs blood tests. Most patients with scarring alopecia benefit by a visit with a dermatologist. it’s true that future appointments and ongoing monitoring may be handled by many different types of specialists, but scarring alopecias are fundamentally dermatological diseases. I understand that it can be difficult to access a dermatologist in many parts of the world. It still does not change the view that dermatologists are the group of physicians with the skills to battle the toughest cases of scarring alopecia.
Treating scarring alopecia is not only about connecting patients with effective treatments but also helping dispel myths and misinformation. Helping patients starts with education – long before I reach for a prescription pad.
Article orginally posted at donovanmedical.com
For more information about cicatricial alopecia, visit carfintl.org
