What is Central Centrifugal Cicatricial Alopecia (CCCA)?
Central Centrifugal Cicatricial Alopecia (CCCA) belongs to a group of disorders called cicatricial or scarring alopecias that destroy the hair follicle, replace it with scar tissue, and cause permanent hair loss. The cause is unknown but is probably an inflammatory process induced by genetic or environmental factors. Women with CCCA develop an area of thinning at the center of their scalp, and this gradually enlarges and spreads outward, hence the name “central centrifugal”. The inflammation that destroys the hair follicle is below the skin surface and there is usually no “scar” seen on the scalp.
Cause
The cause of CCCA is unknown. Genetic factors may be important, and inflammation plays a role in the process. The inflammation, in the form of white blood cells, surrounds the hair follicles and gradually destroys them.
 |
 |
 |
Signs & Symptoms
CCCA affects primarily women of African descent, but rarely occurs in women of other ethnic groups and men. It usually presents in individuals 25-65 years of age. There have been several reports of CCCA occurring in families and genetic studies are currently underway to further identify possible contributing genes. However, most patients with CCCA have no family history of a similar condition. CCCA is not associated with any other illnesses.
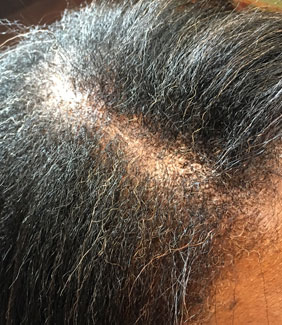
In many cases, the area of hair loss of CCCA is not accompanied by any symptoms. In some cases, the hair loss is associated with itching, burning, tenderness, pain or a tingling sensation. The bare area gradually enlarges and may affect a large portion of the central scalp with only few solitary hairs remaining. Two other hair problems, hair breakage and traction alopecia (hair loss along the hairline), may be present in some women with CCCA, but it is not clear if they are at all related to the scarring process. Hair breakage and traction alopecia are both due to hair styling and hair grooming practices and the relationship to the development of CCCA is still being determined.
Diagnosis & Treatments
Experienced dermatologists will suspect the diagnosis of CCCA from a detailed clinical history, thorough physical examination of the scalp, and scalp biopsy. A scalp biopsy the gold standard of diagnosis of scarring hair loss and are often performed when considering a diagnosis of CCCA. The biopsy procedure is performed in the office with a local anesthetic, and a small skin sample is taken for microscopic examination. The most helpful information from the biopsy is the extent of inflammation, number of hair follicles present, and the amount of scar tissue, which are all used to select appropriate therapy.
Early diagnosis and therapeutic intervention can often prevent permanent damage to hair follicles. Once a definitive diagnosis is made, we can determine the best treatment plan for each individual. Some regrowth is even possible with treatment.
The goals of treatment are to relieve symptoms, signs, and halt spread of the disease. Hair regrowth is not possible after the hair follicles are replaced by scar tissue. For this reason, it is important to start treatment early before the hair loss is extensive.
Treatments include anti-inflammatory medications to decrease the inflammation surrounding the hair follicle and prevent its permanent destruction. In mild cases, topical corticosteroids in the form of ointments, oils, solutions, lotions, foams, sprays or shampoos can help decrease inflammation and calm associated symptoms (itching, redness, or pain). Topical tacrolimus may also be helpful as a steroid sparing topical agent. Additionally, injections of corticosteroid, such as triamcinolone acetonide, may be used in inflamed and symptomatic areas, every 4-6 weeks. In more advanced cases, the addition of oral medications is needed such as tetracycline antibiotics (used for its anti-inflammatory properties), or hydroxychloroquine (an antimalarial drug with anti-inflammatory properties). Topical minoxidil may be useful in the form of solution or foam to keep the remaining follicles in their growing phase longer and stimulate longer hair growth. Hair transplantation is an option only in selected cases and after the inflammation has been controlled and hair loss is no longer spreading.
Women with CCCA should handle their hair gently and may continue to use their usual shampoo and conditioner if there is no breakage or traction alopecia. When hair breakage is present, the hair is short and seems to have “stopped growing”. It is then important to avoid excessive heat and chemical processing. Perms and relaxers should also be minimized, and the interval between them increased to 8 weeks or longer. A hair piece or wig is a good way to give hair a rest from heat and chemicals. When traction alopecia is present, avoid pulling hair styles such as tight ponytails; braids and corn rows should be loose and not pulled tightly at the scalp; heavy hair extensions should be avoided.
What is cicatricial alopecia or scarring alopecia?
Cicatricial alopecia refers to a group of rare disorders with a highly variable course
The term “cicatricial alopecia” refers to a diverse group of rare disorders that destroy the hair follicle, replace it with scar tissue, and cause permanent hair loss. The clinical course is highly variable and unpredictable. Hair loss may be slowly progressive over many years, without symptoms, and unnoticed for long periods. Or the hair loss may be rapidly destructive within months and associated with severe itching, pain and burning. The inflammation that destroys the follicle is below the skin surface and there is usually no “scar” seen on the scalp. Affected areas of the scalp may show little signs of inflammation, or have redness, scaling, increased or decreased pigmentation, pustules, or draining sinuses. Cicatricial alopecia occurs in otherwise healthy men and women of all ages, is not contagious, not hereditary and is seen worldwide.
Are there different kinds of cicatricial alopecia?
This brochure discusses primary cicatricial alopecias in which the hair follicle is the target of the destructive inflammatory process
Yes, cicatricial alopecias are classified as primary or secondary. This discussion is confined to the primary cicatricial alopecias in which the hair follicle is the target of the destructive inflammatory process. In secondary cicatricial alopecias, destruction of the hair follicle is incidental to a non-follicle-directed process or external injury, such as severe infections, burns, radiation, or tumors.
Primary cicatricial alopecia is currently classified by the type of inflammatory cells seen on scalp biopsy. The inflammatory cells may be primarily lymphocytes, neutrophils, or sometimes the inflammation has mixed cells. Cicatricial alopecias that involve predominantly lymphocytic inflammation include lichen planopilaris, frontal fibrosing alopecia, central centrifugal cicatricial alopecia, pseudopelade (Brocq), chronic cutaneous lupus erythematosus, and keratosis follicularis spinulosa decalvans. Cicatricial alopecias that involve predominantly neutrophilic inflammation include folliculitis decalvans and tufted folliculitis. Sometimes the inflammation shifts from a predominantly neutrophilic process to a lymphocytic process, or visa versa. Cicatricial alopecias with a mixed inflammatory infiltrate include dissecting cellulitis and folliculitis keloidalis, both of which are secondary to follicular rupture.
What causes cicatricial alopecia?
New research suggests that there is a loss of function of a “master regulator”
The cause of the various cicatricial alopecias is poorly understood. However, all cicatricial alopecias involve inflammation directed at the hair follicle, usually the upper part of the follicle where the stem cells and sebaceous glands (oil gland) are located. If the stem cells and the sebaceous glands are destroyed, there is no possibility for regeneration of the hair follicle and permanent hair loss results.
Research suggests that there is a loss of function of a “master regulator” called the peroxisome proliferator-activated receptor gamma, or PPAR gamma. PPAR gamma plays an important role in the preservation of hair follicle cells, including stem cells, and sebaceous glands. Decreased PPAR gamma leads to a sebaceous gland dysfunction, which causes abnormal processing and buildup of “toxic” lipids. This abnormal buildup of lipids triggers inflammation that ultimately destroys the hair follicle.
Who is affected by cicatricial alopecia?
Cicatricial alopecias affect both men and women of all ages and are rare in children
Cicatricial alopecias affect both men and women of all ages and are rare in children. Some disorders may manifest in the teenage years. Epidemiologic studies have not been performed to determine the incidence of cicatricial alopecias. In general, they are not common.
There have been a few reports of cicatricial alopecia occurring in a family. However, the majority of patients with cicatricial alopecia have no family history of a similar condition.
Central centrifugal cicatricial alopecia women of African ancestry most commonly and may occur in several family members. Frontal fibrosing alopecia is seen most commonly in post-menopausal women but also occurs in young women and men. While it is possible to have more than one type of hair loss condition, non-scarring types of hair loss do not turn into scarring forms of hair loss.
Are cicatricial alopecias associated with other illnesses?
In general, cicatricial alopecias are not associated with other illnesses and usually occur in healthy men and women.
Patients with chronic cutaneous lupus erythematosus may have an increased personal and family history of autoimmune disorders.
How are cicatricial alopecias diagnosed?
A scalp biopsy is the essential first step in diagnosing a cicatricial alopecia
A scalp biopsy is essential for the diagnosis of cicatricial alopecia and is the necessary first step. Findings of the scalp biopsy, including the type of inflammation present, location and amount of inflammation, and other changes in the scalp, are necessary to diagnose the type of cicatricial alopecia, to determine the degree of activity, and to select appropriate therapy.
Clinical evaluation of the scalp is also important. Symptoms of itching, burning, pain or tenderness usually signal ongoing activity. Signs of scalp inflammation include redness, scaling, and pustules. However, in some cases there are few symptoms or signs and only the scalp biopsy demonstrates the active inflammation. The overall extent and pattern of hair loss is noted and sometimes photographed for future comparison. A hair “pull test” may be performed to identify areas of active disease in which hairs are easily pulled out. In addition, if pustules are present, cultures may be performed to identify which microbes, if any, may be contributing to the inflammation. A thorough evaluation that includes all of these parameters is important in diagnosing a cicatricial alopecia and in identifying features in individual patients that will help the selection of therapy.
Diagnosis and treatment of cicatricial alopecias is often challenging. For this reason, it is helpful to be evaluated by a dermatologist with a special interest or expertise in scalp and hair disorders, and who is familiar with current diagnostic methods and therapies. A hair specialist who is experienced in the evaluation and treatment of patients with cicatricial alopecias may be found by contacting the Cicatricial Alopecia Research Foundation, the American Academy of Dermatology , or the North American Hair Research Society.
How are cicatricial alopecias treated?
Treatment strategies differ depending on the types of inflammatory cells that are attacking the hair follicles
As mentioned above, primary cicatricial alopecias are classified by the predominant type of inflammatory cells that attack the hair follicles: i.e., lymphocytes, neutrophils, or mixed inflammatory cells. Treatment strategies are different for each of these three subtypes and detailed treatment options are beyond the scope of this discussion.
However, certain general principles are reviewed below.
Treatment of the lymphocytic group of cicatricial alopecias involves use of anti-inflammatory medications
Treatment of the lymphocytic (including lichen planopilaris, group of frontal fibrosing alopecia, cicatricial alopecias central centrifugal cicatricial alopecia, pseudopelade (Brocq), chronic cutaneous lupus erythematosus, and keratosis follicularis spinulosa decalvans) involves use of anti-inflammatory medications. The goal of treatment is to decrease or eliminate the lymphocytic cells that are attacking and destroying the hair follicle. Oral medications may include hydroxychloroquine, doxycycline, mycophenolate mofetil, pioglitazone, cyclosporine, or corticosteroids. Topical medications may include corticosteroids, topical tacrolimus, Derma-Smoothe/FS scalp oil; triamcinolone acetonide (a corticosteroid) may be injected into inflamed, symptomatic areas of the scalp.
Treatment of the neutrophilic group of cicatricial alopecias is directed at eliminating the predominant microbes
Treatment of the neutrophilic group of cicatricial alopecias (folliculitis decalvans and tufted folliculitis) is directed at eliminating the predominant microbes that are invariably involved in the inflammatory process. Culture and sensitivities are essential for the selection of oral antibiotics, which are the mainstay of therapy. Topical antibiotics may be used to supplement the oral antibiotic and triamcinolone acetonide (a corticosteroid) may be applied or injected into inflamed areas.
Treatment of the mixed group may include antimicrobials, isotretinoin, anti-inflammatory medications, and tumor necrosis factor inhibitors
Treatment of the mixed group of cicatricial alopecias (dissecting cellulitis and include folliculitis keloidalis) may include antimicrobials although culture often does not grow a pathogen. Isotretinoin, anti-inflammatory medications such as corticosteroids, and tumor necrosis factor inhibitors may be used. In dissecting cellulitis, incision and drainage of nodules may be needed.
You should discuss any treatment with your dermatologist who will also explain potential side effects, as well as laboratory tests that are needed before starting medications and sometimes are monitored during treatment.
Treatment is continued until the symptoms and signs of scalp inflammation are controlled
The course of cicatricial alopecia is usually prolonged and treatments are often given for 6 to 12 months or longer. Treatment is continued until the symptoms and signs of scalp inflammation are controlled. In other words, itching, burning, pain and tenderness have cleared and scalp redness, scaling, and/or pustules are no longer present.
Treatment may then be stopped. However, with the exception of pioglitazone, current treatments do not usually influence the underlying process and may not arrest progression of hair loss even when symptoms and signs have cleared. Clinical activity often recurs and treatment frequently needs to be repeated.
Because of the above last statement, surgical treatment is not an option in most cases except under certain circumstances. If the disease has been inactive for one or two years, then surgical removal of the scarred scalp and/or hair restoration surgery may be considered for cosmetic benefit. Folliculitis keloidalis is one exception in that excision of the affected scalp (scalp reduction) may provide relief for the patient.
Will my hair grow back?
Begin treatment as early as possible to halt the inflammatory process and follicle destruction
Hair will not regrow once the follicle is destroyed. However, it may be possible to treat the inflammation in and around the surrounding follicles before they are destroyed and for this reason it is important to begin treatment as early as possible to halt the inflammatory process. Minoxidil solution (2% or 5%) applied once (5%) or twice (2%) daily to the scalp may help to stimulate any small, remaining, unscarred follicles. The progression of hair loss is unpredictable. In some cases, progression is slow and there is sufficient hair remaining to cover the affected scalp areas; in other cases, progression can be rapid and extensive.
How should I care for my hair?
Hair care products and shampoos can generally be used with any frequency desired, as long as the products are not irritating to the scalp. Dermatologists may recommend specific shampoos and products to decrease scalp symptoms, scaling, and inflammation. Hair pieces, wigs, hats, scarves may be used freely. Check out THIS ARTICLE to learn more about what ingredients to aviod in your hair care products.
